Endodontic Microsurgery (‘Apicectomy’)
Occasionally, conventional root canal treatment (through the top of the tooth) may not work or can not be performed, despite the best efforts of a Specialist endodontist.
Reasons for this might be:
- Attempting to re-treat a previous root canal filling has a statistically lower success rate of 70-80% (compared to 95% success if it was performed properly the first time round).
You can catch a short video on endodontic re-treatment below. - Re-treating the root canals from the ‘top’ of the tooth may be too destructive to the existing crown or bridgework
- Cleaning of the root canals may be technically extremely difficult or impossible due to a blockage or calcification
- Long-standing infection may be resistant to conventional root canal treatment. This is due to infection surviving outside the end of the roots. This will then require a direct surgical investigation and removal
Unfortunately, the only other way to eliminate infection that persists at the end of the root(s) is by extraction of the tooth.
Your general dentist can explain to you all the reasonable options and alternatives to surgery and the Specialist endodontist can inform you of the success rate and costs of the surgery.
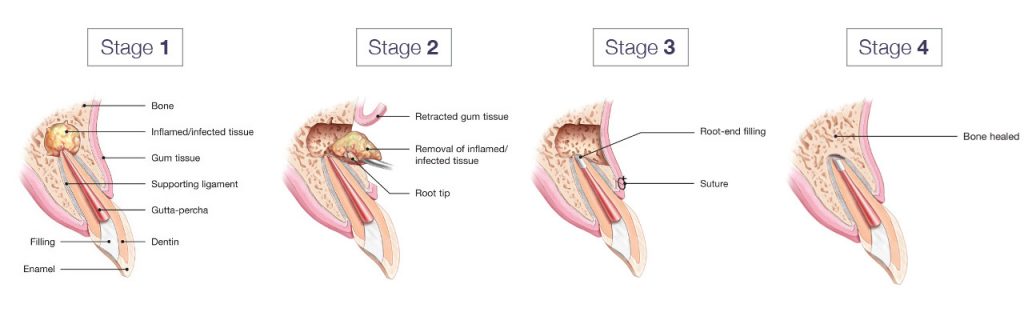
Essentially, the overlying gum tissue over the site of the root infection is peeled back so direct access is made to visualise the infected tissue. The tissue is then removed together with the infected root-end. A small root filling is then placed back into the root canal to seal the root, and the gum tissues are stitched back so that they can heal normally.
Over the first few weeks the gums will heal back to their normal appearance and over a period of months, the bone will heal round the end of the roots.
You can also see the stages of this procedure here, with images courtesy of the AAE, “Your guide to Endodontic Surgery”:
For more information on the procedure please see the video here:
The whole procedure is performed under local anaesthetic so that everything around the tooth is numb and you will not feel any pain. When the anaesthetic has worn off and for a few days after the procedure, there will be some soreness in the gums.
Evidence shows that taking an anti-inflammatory just before and after the treatment (e.g. 400 mg ibuprofen, “Nurofen Plus”), or if you have a medical condition that precludes you taking his type of painkiller (e.g. asthma, gastric ulcer) then 1000mg Paracetomol will help minimise the discomfort.
The endodontist will then review you again within the first a week to remove the stitches. The tooth will be reviewed again after 6 months assess how well the bone has healed at the end of the root.
Immediate Post-treatment Care Guides
For the first few days after treatment the tooth may feel a little ‘achy’, especially if there was pain or infection before the procedure.
This discomfort is sometimes caused by the fact that we have instrumented and disturbed the infected area just outside the end of the roots and the pressure of applying the root-filling. This can be relieved with over-the-counter or prescription medications.
Evidence shows that taking an anti-inflammatory just before and after the treatment (e.g. 400 mg Ibuprofen, “Nurofen Plus”), or if you have a medical condition that precludes you taking his type of painkiller (e.g. asthma, gastric ulcer), then 1000mg Paracetomol will help in minimising the discomfort.
If you have had Endodontic Microsurgery (Apical Surgery), download Endo61 post-treatment information here: